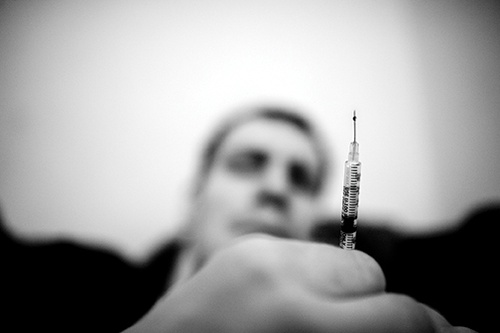
 Mike, a client of Insite, prepares a syringe.
Photograph by Simon Hayter.
Mike, a client of Insite, prepares a syringe.
Photograph by Simon Hayter.
Best Shot
Vancouver’s Insite is an unqualified success. So why is it still the only supervised- injection clinic in North America?
AT 139 EAST HASTINGS STREET,
soft music plays as drug users
hunker in front of full-length
mirrors and stainless-steel sinks. Under the watchful eyes of nurses, they
inject themselves with heroin and cocaine. Twelve booths, each with overhead lighting, create the impression of
a backstage dressing room. Tacked to
the message board in the cluttered staff
office is a hand-written note: “Hello
everyone. I just wanted to say, over 400
recovered overdoses in the first year.
So I say ‘wow’. Thanks ever so much
cause I was one of those people! From Richard (aka Sum Asso).”
In the nearly ten years since Richard left this note, Insite, the East Vancouver safe-injection clinic, has had more than a million visits and not a single overdose death. It has won the grudging support of local police, the backing of the medical establishment and, after the Harper government tried to shut it down, a landmark Supreme Court case.
But, despite its success, Insite remains the only safe-injection site in North America. The mayors of Toronto, Ottawa and Montreal have recently shot down proposals for similar clinics, and a new law tabled by the federal government, the Respect for Communities Act, will give more veto power to local officials and police chiefs. While Insite may have won its fight, the debate surrounding supervised-injection sites is far from over—and the battle lines have shifted east.
FOR ALL THE ATTENTION it’s received in its decade-long history, Insite is an unassuming place. Located in the Downtown Eastside neighbourhood, between a boarded-up rooming house and a store called Adult Merchandise, the clinic’s front window displays a modest-sized decal of a cartoon needle. A banner hanging over the front door reads “Insite Saves Lives.” About a thousand visitors walk through the entrance every day, 365 days a year.
While the main function of the clinic is still to prevent overdoses—nurses hover behind patients as they inject, to make sure they don’t “nod off”—there is also a twelve-bed treatment centre upstairs called Onsite. Insite also acts as a first point of contact between drug users and the health-care system. “People can come in here to have an abscess treated, or to have a warm cup of coffee, or just to make a phone call,” says head clinician Bethany Jeal. They also stop by to pick up clean needles, condoms and band-aids.
Today, most Vancouverites are in favour of Insite—nearly 70 percent, according to recent surveys. But it wasn’t always that way. When it was first proposed, the idea of providing a place for junkies to shoot up didn’t go over well with local business owners in nearby Chinatown and Gastown. Even neighbourhood drug users weren’t so sure. Mark Townsend is the co-founder of the Portland Hotel Society, which operates Insite with Vancouver Coastal Health. He recalls talking to addicts about the idea in the mid-1990s. They thought he was crazy. “I remember thinking that if even the users don’t support it, there’s not much hope with the public,” Townsend tells me.
At the time, the Downtown Eastside was bottoming out. The arrival of China White heroin and crack cocaine in the early 1990s wreaked havoc. By 1997, according to some estimates, the HIV rate in parts of the neighbourhood had reached 30 percent. Townsend says that overdose deaths in the ubiquitous single-occupancy hotel rooms were almost inevitable. “In the realm that we were living, it was like a dead cat—they’d get whisked off and that was the end of it,” he recalls.
Desperate for answers, advocates and health experts began looking overseas. In the Netherlands, a handful of supervised-injection sites had opened in the 1970s. Germany and Switzerland later followed suit; there are now an estimated ninety safe-injection sites in eight countries. Some experiments failed, but most of the European facilities showed encouraging results—and sparked a movement for a similar site in Vancouver.
Gathering support for the idea meant years of educating the community and politicians. “That’s the crux that always gets missed,” says Townsend. “It took a massive amount of work.” Larry Campbell, a former chief coroner of BC and the inspiration behind CBC televi- sion’s Da Vinci’s Inquest, was an early skeptic. To him, the notion of helping drug addicts get their fix seemed counterintuitive. But, as the death toll kept rising, he realized that the old approach of arresting drug addicts—or simply ignoring them—wasn’t working.
In 2002, Campbell ran for mayor, promising to open Insite within three months of his election. He won by a landslide. It took nine months longer than he’d hoped, but, when the clinic’s doors finally opened in September 2003, some six hundred users showed up. “When you look at it now,” says Campbell, today a Liberal senator, “there’s nothing controversial about it. It’s a health clinic.”
BUT, ELSEWHERE IN CANADA, safe-injection sites still create conflict. Six years ago, Chris Grinham and his wife discovered a used needle in their Ottawa neighbourhood. Soon after, the couple founded Safer Ottawa, an organization promoting drug treatment, prevention and education surrounding drug use. Safer Ottawa is opposed to what it calls “consumption sites.” “It’s really misleading to call them ‘safe-injection’ sites,” Grinham tells me. “There’s absolutely nothing safe about injecting those kinds of substances into your body.”
Outside of Vancouver, Ottawa has the highest HIV transmission rate among drug users in Canada. Between three and four thousand injection-drug users live here, and public drug use is on the rise. Grinham, who has picked up more than six thousand needles in his Lowertown neighbourhood, admits that he’s not an addictions expert—he’s an IT guy. But he’s done his homework, he says, and the more he’s learned about injection sites, the more opposed he’s become. “Within a certain radius, the drug laws don’t exist, and that becomes a huge attractant— not just for drug use, but for dealers,” he says. “If they were to put one here in Ottawa, it would literally destroy that part of town.”
But supporters of safe-injection clinics have science on their side. Over thirty papers have been published about Insite in medical journals, including the Lancet, the New England Journal of Medicine and the Canadian Medical Association Journal. The results have been unanimously supportive: a 35 percent reduction in overdose deaths in the area, lower blood-borne disease transmission rates and a measurable increase in the number of users seeking treatment. While many share Grinham’s perception that safe-injection sites produce a honey-pot effect and increase crime, that hasn’t been the case at Insite, where crime rates have remained relatively unchanged. And a recent study done by researchers at the University of Toronto and St. Michael’s Hospital recommended that the Insite model spread elsewhere in Canada, suggesting the creation of three sites in Toronto and two in Ottawa.
STILL, IN THOSE CITIES, the fight for safe-injection sites is just beginning. Under the Respect for Communities Act, the federal health minister has carte blanche to deny applications if local mayors and police chiefs don’t support such clinics.
Dr. Mark Tyndall, the head of infectious diseases at the University of Ottawa and a former researcher at Vancouver’s HIV Centre for Excellence, is part of a volunteer group preparing an application for an injection site in Ottawa. He argues that these clinics should be a matter of public health, not local politics. “If we need to get the mayor to sign a letter saying he supports this, then it won’t happen here,” he says. “It’s a dagger through anybody’s hope of opening a site.”
Despite the challenges, Tyndall’s group is aiming to have an application to the federal health minister by the end of the year. The Cactus Montreal needle exchange is also planning to submit an application for an injection site soon. Previous Montreal mayors would only support one if it were located in an existing health-care facility; advocates, on the other hand, argued that Montreal’s hospitals are too far from heavy drug-use areas to be effective. “I really think that the right thing will eventually prevail and we’ll have more sites running,” says Tyndall. “But it’s taking far too long. People are dying while we wait to get things together."
According to Campbell, the most difficult myth to overcome is the idea that injection sites somehow enable drug addiction. “I’ve never met an addict yet that’s glad they’re an addict,” he says. The addicts are out there, and they’re going to shoot up anyway. A clinic, if nothing else, can prevent deaths.
ON MY LAST VISIT TO INSITE, I meet Richard. We sit in the clinic’s back office, below the thank-you note he penned all those years ago. Since then, he tells me, he’s had a few more near-death experiences here. A nasty leg infection almost killed him, until clinic staff saw to it that he got daily treatment at St. Paul’s hospital; sometimes, they even arranged for taxis to get him there. Richard talks in the jargon of a hardened drug user, using words like “half-caps” and “cookers” and “juggers,” and his stories begin to bleed together after a while—brushes with death, revivals and relapses.
Richard is thirty-eight years old. He collects bottles for a living. He’s never been to treatment, but, unlike in his earlier years, when he would inject $75 in speed and heroin and binge for days on end, he now visits the clinic like clockwork, injecting only enough to satisfy his addiction, to keep it at bay. If drugs were ever a party for Richard, that party ended long ago. For now, he seems to be circling around his addiction, like a wrestler sizing up his opponent.
Toward the end of our talk, I ask him why people should care whether he lives or dies. It is, after all, the central question in this whole debate. How much taxpayer compassion does a drug addict ultimately deserve? Richard pauses for a moment, unsure how to answer. “I’m human,” he finally says. “I don’t blame anyone, society, for where I am. I’ve made mistakes, but I’m a human being."





